Diaries of 24 Viruses: How long they are asymptomatic, when & what symptoms appear first, and what can we learn.
Chart 1:
Our Chinese colleagues have published an important paper recently. The first chart shows 24 rows, each row an individual patient. The vertical brown line is the day of diagnosis. The gray boxes on the left, labelled with negative numbers along the top, are asymptomatic days before the diagnosis. They end backwards in time on the day of the probable infection.
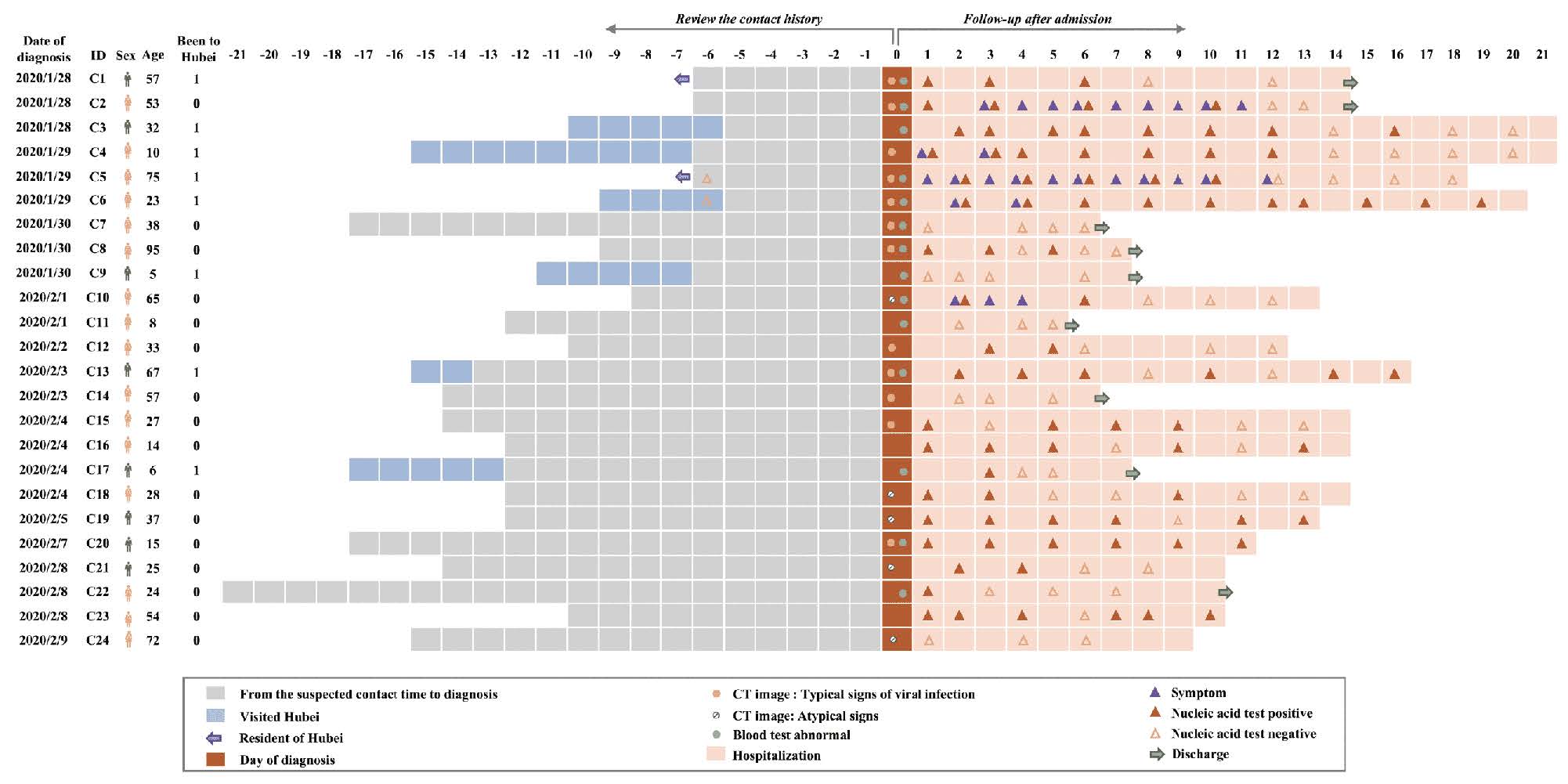
This can never be known for sure of course, but this is a standard way to do this research. The beige color are the days in the hospital. Symbols are various tests done along the way. Their meaning is on the bottom.
Learnings:
1. It took 7 to 21 days from exposure to a clinical diagnosis of the virus.
2. Two patients, C5 and C6, had NEGATIVE DNA tests during that time, the one everyone wants to take. So in these patients the test was done too early (24 to 72 hours after exposure) and came back negative. They could have gone out and partied, thinking they could not transmit the disease.
3. I love patient C8! She’s a 95 year old woman who has symptoms, tests positive for 5 days, tests negative for two days, and is discharged on day 7! So there, virus; Girl Power!
3. Patient C4 and C9: A 5 year old boy and a 10 year old girl. So this DOES infect kids. School closings noted. Also, the 10 year old spent 21 days (and still there at time of publication) in the hospital, so, not a walk in the park for her.
4. The arrow at the right end is a patient cured, going home. Only 9 of 24 were discharged at the time of the paper and some are in the hospital for three weeks and beyond. This slow recovery impacts resources of course.
Chart 2:
This is a kind of worse case scenario, all in one family. Case 13 from the below table. The husband spent 48 hours in Hubei, where he picked up the disease. He then returned to his family, a wife, son, and daughter-in-law.
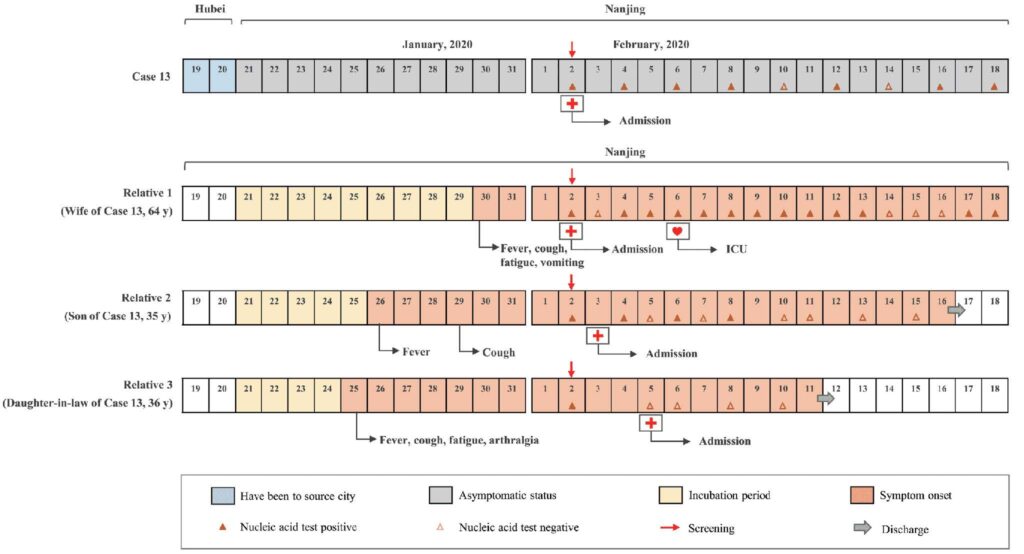
Learnings:
1. The husband, 67 years old, NEVER had any symptoms. He was admitted because of what happened to his family. And the DNA test, the ‘Gold Standard’ was positive four times in a row over six days, and then was NEGATIVE twice and positive twice. Why the variability? When you have no symptoms you have very little virus so you don’t test positive for it but you sure can pass it on.
SO YOU CAN TRANSMIT THIS DISEASE WITH SO FEW VIRUS COPIES THE DNA TEST IS NEGATIVE.
2. The wife, age 64, had a fever and cough three days before admission, tested positive on admission, and rapidly deteriorated and went into the Intensive Care Unit. She remained in serious condition at the time of publication.
3. The 35 y son had a fever and cough eight and five days, respectively, before the DNA test was positive. His DNA test was negative within five days of hospitalization and he was discharged after 16 days. So focus; a GOOD outcome for a patient who gets in the hospital is a 16 day stay. A resource problem.
4. His wife, age 36, had a fever and cough eight days before a positive DNA test, spent six days in the hospital and. went home healthy.
FINAL LEARNING:
A screening test should be quick, easy, cheap, give fast answers, and be highly sensitive.
That is, if I ask God to be my lab assistant (in medical jargon, absolute truth against which a test is going to be compared) and to give me 100 known coronavirus patients one week from being sick enough to go to the hospital, how many of that 100 can I pick up with my test? Combining other studies here tells me that 90 of these patients, one week before hospitalization, had either a fever or could not hold a big breath for 10 seconds without coughing.
So turning it upside down, if you pass both tests, you have only a 10% chance of being sick next week. It might be that the 10% are going to be like Case 13, who never had a symptom, but who are silent carriers. In this case only God knows they are sick.
So checking breath hold and temp, with 90% sensitivity, is not bad for two tests that are free and take less than 2 minutes!
Reference for above: https://link.springer.com/artic…/10.1007%2Fs11427-020-1661-4




